When OASIS submission, coding, and QA review were streamlined, Qavalo’s client agencies saw significant improvements in their OASIS turnaround time and realized better compliance and profitability.
With the right outsourcing partner, Qavalo clients have been able to get the support their in-house teams need to find efficiencies in their documentation workflow and seize big picture process improvement opportunities.
Benefits Realized
- Consistent OASIS submission-to-completion process
- Faster OASIS submission time
- Shorter OASIS turnaround time
- Declining LUPA rates
- Optimized reimbursement values
PDGM Turnaround Time Challenges
The Patient-Driven Groupings Model (PDGM) overhauled the entire home health reimbursement system with new case-mix weight calculations, new LUPA thresholds, new Request for Anticipated Payment (RAP) requirements, and shorter payment periods, among other big changes.
Request for Anticipated Payment (RAP)
In 2020, CMS introduced RAP, requiring agencies to submit initial documentation to authorize care under a home health agency and establish the care episode. Though a complete OASIS is no longer a requirement to file a No-Pay RAP this year, it is still best for agencies to complete the OASIS within the 5-day window period.
HHRG and HIPPS codes
Based on an OASIS assessment, 30-day periods under PDGM are classified under a variety of patient information and other clinical characteristics, such as admission source, timing, clinical grouping, functional impairment, and comorbidity. This results in a Home Health Resource Group (HHRG) combination for which CMS will generate a PDGM case-mix weight represented as a Health Insurance Prospective Payment System (HIPPS) code on Medicare claims.
Completion of the OASIS in time for RAP filing allows agencies to determine the claim’s HHRG classification and a HIPPS code that is more reflective of the actual patient case. This is important so that the assigned HIPPS code in the RAP would be more consistent with the HIPPS code in the final claim, thus lowering the chance of the agency being flagged for an Additional Development Request (ADR).
Low Utilization Payment Adjustments (LUPA)
With PDGM, LUPA thresholds vary per HHRG over a 30-day period, which means agencies should closely monitor different LUPA thresholds and visit intensities for each patient. Early identification of the LUPA threshold though the HHRG and HIPPS code will help agencies plot and schedule visits accordingly to prevent claims falling under LUPA.
These changes underscore the need for home health agencies to fast-track their process, improve documentation turnaround, and observe strict OASIS completion timelines in order to address key functions that affect claims approvals and reimbursement values. This is no easy task since an OASIS needs to undergo a number of processes, including coding and QA review, before being completed. In many cases, this can take up to 10 days—or ⅓ of the care period—if processes are not streamlined.
Qavalo Solutions in Numbers
To address the abovementioned challenges, Qavalo applies several workarounds and best practices to help agencies achieve the ideal workflow and succeed in timely submissions.
- Timely coding and OASIS review to allow agencies to identify LUPA thresholds ahead of time, and generate a HIPPS code that is reflective of the actual patient case.
- Coding is done as soon as the OASIS is available in the QA manager.
- Coders are available seven (7) days a week.
- OASIS QA review is completed within 48 hours after coding.
- There is efficient resolution of escalations of OASIS quality issues.
- Qavalo proactively notifies agencies of trends on late submissions of OASIS by the clinicians.
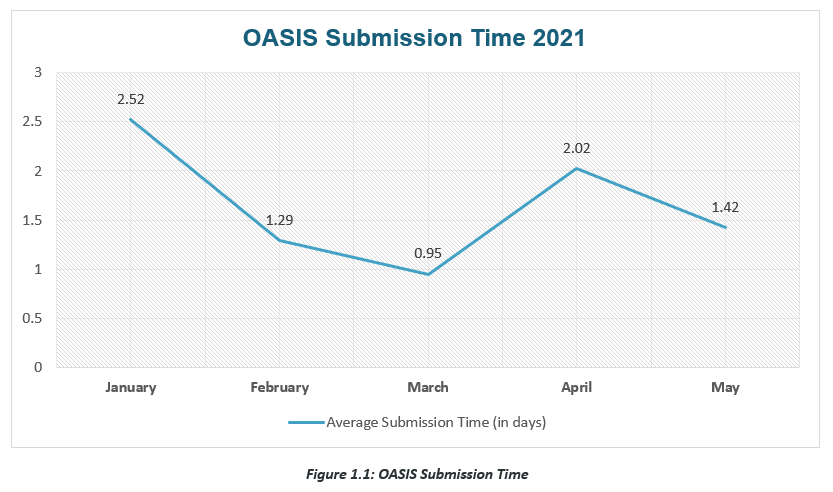
Figure 1.1 shows the average OASIS submission time of clinicians across all home health agency clients of Qavalo. In January 2021, average OASIS submission was at 2.52 days, and by May 2021, this decreased to only 1.41 days.
More importantly, figure 1.2 below shows the average OASIS turnaround time from clinician submission to final approval. From January to May of 2021, Qavalo home health agency clients were able to realize completion of the OASIS within an average of 3.16 days.
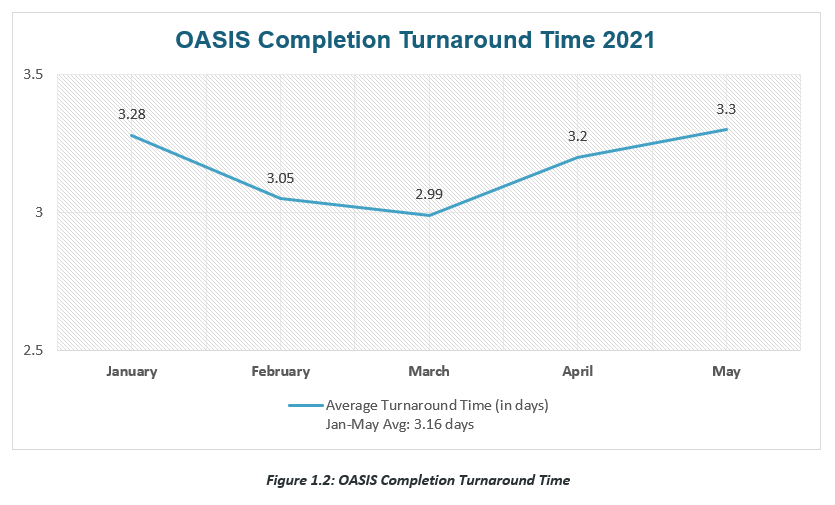 Though a complete OASIS is not required to submit No-Pay RAPs since January 2021, clinicians were able to maintain early submission of OASIS, allowing other OASIS processes, such as coding and QA review, to be accomplished in a timely manner. In addition, Qavalo’s QA review program supports clinician reeducation, helping them improve their charting skills overtime. This resulted in an efficient end-to-end average OASIS turnaround time of 3.16 days, which falls within the 5-day RAP filing window.
Though a complete OASIS is not required to submit No-Pay RAPs since January 2021, clinicians were able to maintain early submission of OASIS, allowing other OASIS processes, such as coding and QA review, to be accomplished in a timely manner. In addition, Qavalo’s QA review program supports clinician reeducation, helping them improve their charting skills overtime. This resulted in an efficient end-to-end average OASIS turnaround time of 3.16 days, which falls within the 5-day RAP filing window.
Due to efficiencies in the OASIS completion timeline, LUPA thresholds were identified early on in the payment period, allowing agencies to properly plot visit schedules, and anticipate and address missed or cancelled visits, thus avoiding LUPAs.
Figure 2 below shows sample data from one of Qavalo’s clients, Palmeria Home Health in Arizona and Nevada. The graph shows the percentage of Palmeira’s LUPA episodes from the fourth quarter of 2020 to the second quarter of 2021.
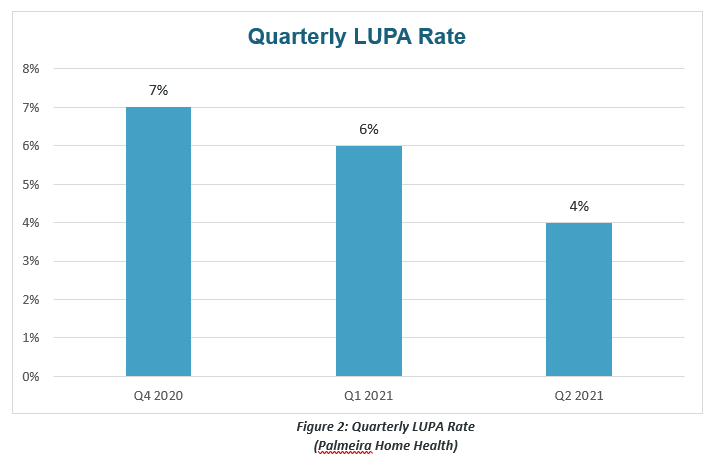
In Q4 of 2020, only 7% of all episodes fell under LUPA. Even with the implementation of No-Pay RAPs in 2021, when the OASIS is no longer required to be completed within 5 days, LUPA rates continued to drop at 6% by Q1 and down to only 4% by Q2.
While early identification of LUPA thresholds greatly helped agencies, LUPAs were not completely avoided because of some uncontrollable factors such as cancelled visits due to patients’ anxiety towards COVID-19.
The Right Partner for the Job
Based on data, Qavalo’s home health agency clients realized a better OASIS turnaround time. Beyond the scope of documentation review and coding, Qavalo maintains ongoing collaboration with in-house teams and leverages data to help agencies have a comprehensive view of their documentation workflow and properly address gaps. This path of progress will only lead to more streamlined processes, resulting in better patient outcomes and business profitability.

